New Approaches to Cancer Treatment Delivery
Cancer care in the United States is increasingly shaped by how treatment is delivered, not only which therapy is chosen. Advances in telehealth, home-based services, outpatient infusion, and coordinated care teams can reduce delays, improve communication, and make complex regimens easier to manage. Understanding these delivery models helps patients and caregivers ask clearer questions and plan for logistics, safety, and follow-up over time.
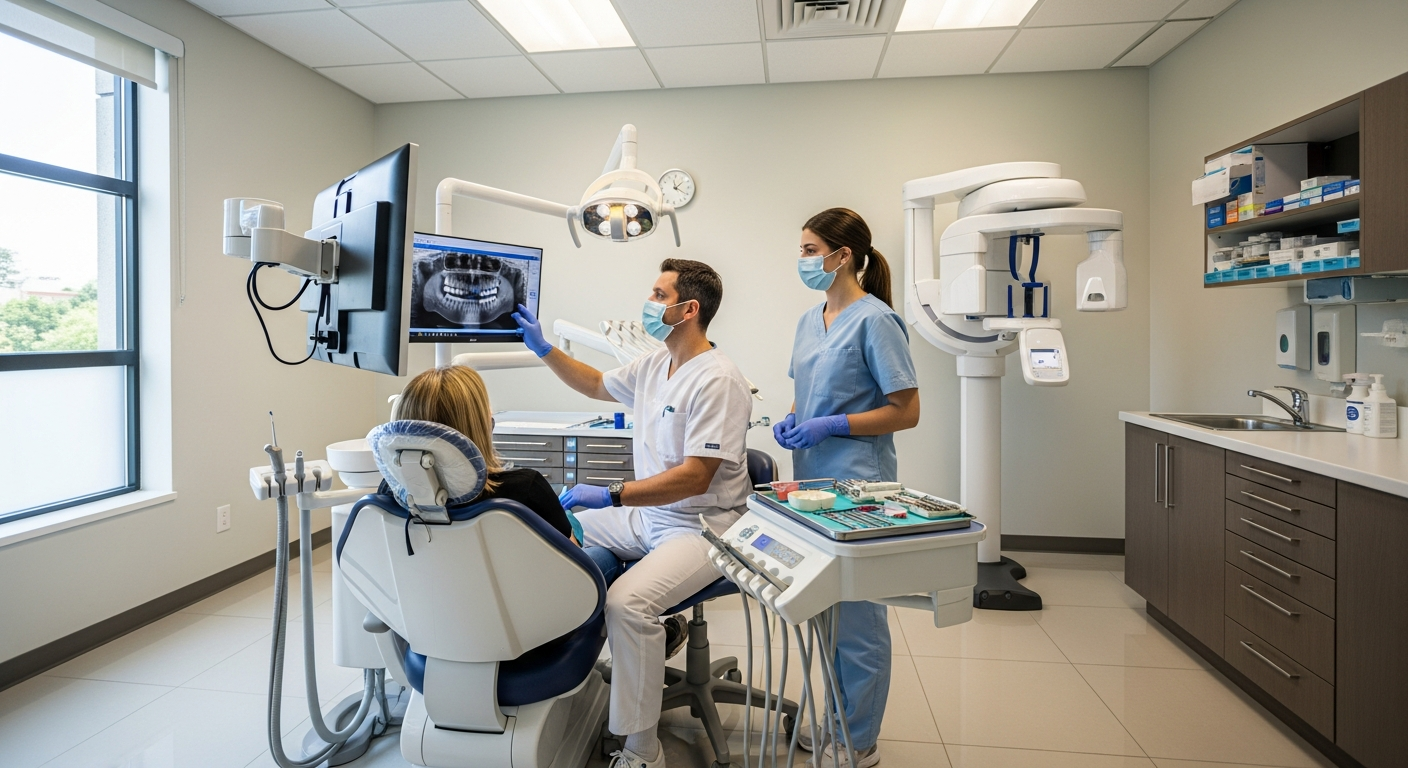
Modern oncology involves more than selecting a medication or procedure; it also requires a reliable system for getting the right care to the right person at the right time. In the U.S., many centers are redesigning workflows so treatment can be delivered closer to home, with fewer unnecessary visits and better coordination among specialists. These changes often focus on safety monitoring, timely symptom management, and practical support for transportation, scheduling, and medication access.
New approaches to treatment delivery in practice
New approaches to delivering cancer treatment often combine digital tools with redesigned clinical pathways. Telehealth visits may be used for treatment planning discussions, side-effect check-ins, nutrition counseling, and some survivorship care, while in-person appointments are prioritized for exams, imaging, infusions, radiation sessions, or procedures that require direct supervision. Many systems also use patient portals, electronic symptom questionnaires, and nurse navigation to flag urgent issues earlier, such as dehydration, fever, or uncontrolled pain.
Another shift is the expansion of outpatient and community-based care when clinically appropriate. Some patients receive supportive therapies (for example hydration, anti-nausea medications, or certain injections) in outpatient clinics that are easier to access than a large hospital campus. For select situations, home-based services—such as mobile phlebotomy, home nursing visits, or remote monitoring—can reduce the burden of travel while still keeping clinicians informed about vital signs and symptoms.
Practical techniques for providing cancer care
Practical techniques for delivering oncology care typically focus on coordination, clear communication, and standardized safety steps. Multidisciplinary tumor boards and shared treatment plans help align recommendations among medical oncology, radiation oncology, surgery, pathology, radiology, genetics, and supportive care. When teams agree on sequencing and timing (for example surgery followed by chemotherapy, or radiation integrated with systemic therapy), patients are less likely to experience avoidable delays.
Standardized protocols can also make delivery safer and more predictable. Examples include medication reconciliation at every transition of care, checklists for central line care, and clear escalation pathways for common complications. Many clinics use proactive symptom management models: patients report side effects between visits, and nurses or advanced practice providers respond with evidence-based guidance. This approach may help prevent emergency department visits by addressing issues early, while still emphasizing that certain symptoms—such as chest pain, shortness of breath, confusion, or high fever—require urgent evaluation.
Access is another practical consideration. Transportation barriers, time off work, caregiver availability, and language needs can affect whether a plan is feasible. Social workers, financial counselors, and patient navigators can support care delivery by coordinating community resources, clarifying insurance requirements, and helping patients understand what to expect before each phase of treatment.
Real-world care delivery models vary by health system, and many organizations combine several approaches—such as telehealth follow-ups, dedicated nurse navigation, clinical trial access, and regional outpatient clinics. The examples below illustrate how established U.S. providers commonly describe their service structures and patient support options.
| Provider Name | Services Offered | Key Features/Benefits |
|---|---|---|
| Mayo Clinic | Multidisciplinary oncology care, telehealth options, clinical trials | Integrated care teams, coordinated specialty referrals |
| MD Anderson Cancer Center | Specialized oncology services, clinical trials, supportive care | High-volume specialty programs, research-driven pathways |
| Memorial Sloan Kettering Cancer Center | Comprehensive oncology care, clinical trials, survivorship programs | Disease-specific teams, extensive supportive services |
| Cleveland Clinic | Cancer services across specialties, regional access points | Coordinated specialty care, broad referral network |
| Kaiser Permanente | Integrated oncology within an insurance/provider system | Coordinated records, streamlined referrals within network |
| Veterans Health Administration (VHA) | Oncology care for eligible Veterans, referrals, supportive services | Integrated system, coordination across VA facilities |
Creative solutions for therapy delivery
Creative solutions for delivering cancer therapy often target the “in-between” moments—what happens outside the infusion chair or procedure suite. Remote symptom monitoring programs can prompt earlier outreach when a patient reports worsening nausea, fatigue, diarrhea, neuropathy symptoms, or mood changes. Some systems add pharmacist-led medication management to help with oral therapies, adherence challenges, drug interactions, and side-effect mitigation.
Another innovation is shifting appropriate services to lower-intensity settings without compromising oversight. Examples can include “hospital-at-home” models for select supportive interventions, or partnership clinics that provide infusions or lab work in your area under standardized protocols. For rural communities, hybrid schedules—alternating in-person visits with telehealth—may reduce travel while preserving periodic physical exams and imaging. These models work best when roles are clearly defined (who to call after hours, where labs are drawn, how results are communicated) and when there is a plan for urgent escalation.
This article is for informational purposes only and should not be considered medical advice. Please consult a qualified healthcare professional for personalized guidance and treatment.
Improving how treatment is delivered can make cancer care more responsive, safer, and easier to navigate—especially when multiple therapies and appointments are involved. By understanding emerging delivery models such as coordinated care teams, telehealth-supported follow-up, outpatient and community-based services, and proactive symptom monitoring, patients and caregivers can better anticipate logistical needs and discuss practical options with their clinical team.