Key Points About Screwless Dental Implants You Might Not Have Considered
Screw-retained restorations get a lot of attention, but so-called “screwless” implant teeth raise different practical questions. From how the crown is attached to what happens during maintenance, the details can affect cleaning, gum health, and future repairs. Understanding the trade-offs can help you discuss options more clearly with your dental team.
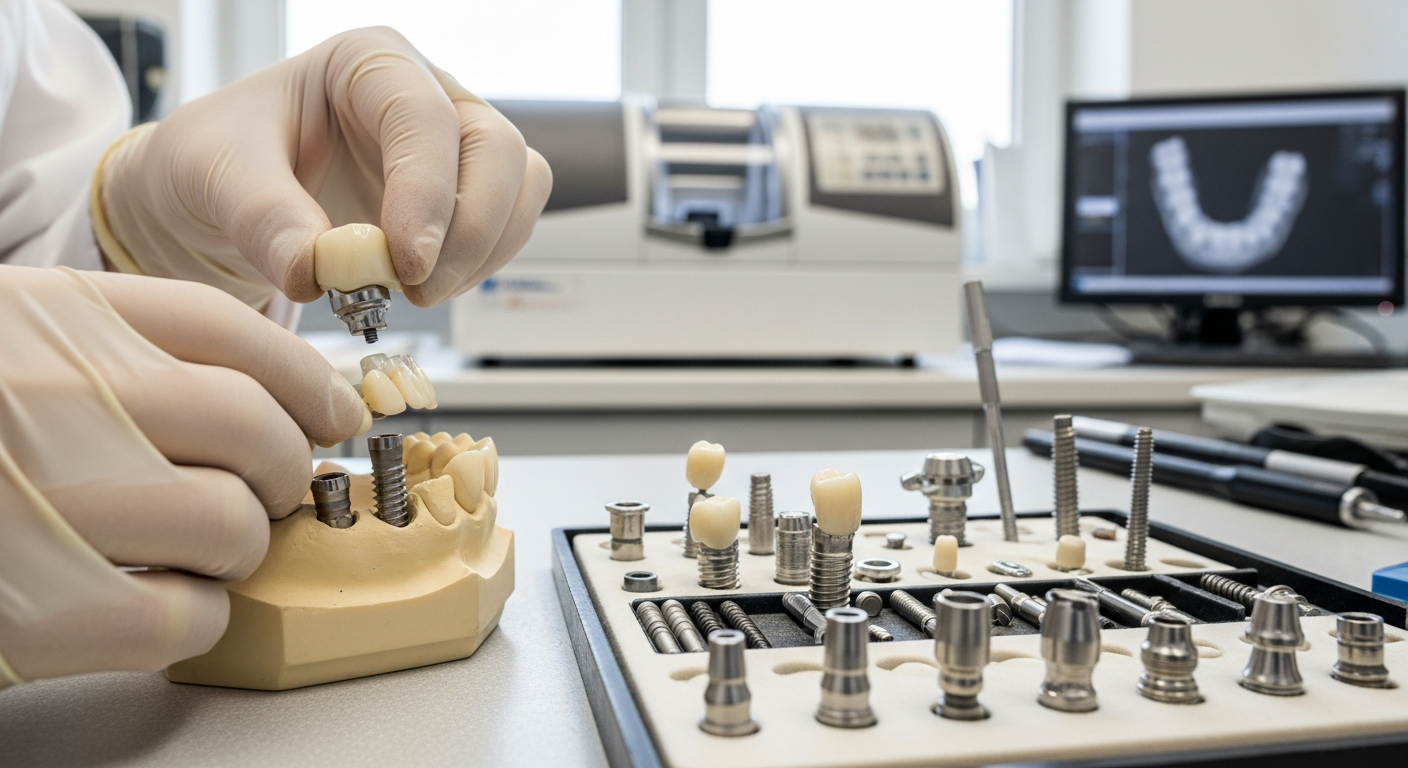
Modern implant restorations are often described in simple terms—“with a screw” or “without a screw”—but the reality is more nuanced. In many U.S. dental practices, “screwless” commonly refers to restorations that do not show or use an access screw through the biting surface, even though a screw may still exist at a deeper connection. The way a crown is attached influences appearance, the ability to retrieve the restoration later, and the steps needed to manage complications.
Screwless Dental Implants: what “screwless” can mean
The phrase Screwless Dental Implants is usually shorthand for an implant crown that is not held in place by a visible occlusal (biting-surface) screw channel. In practice, this often points to a cemented crown over an abutment, or to newer approaches that hide the retention method (for example, angulated screw channels or systems designed to mask access openings). The key is to clarify what part is “screwless”: the crown may be cemented to an abutment that is itself secured to the implant with a screw.
The trade-off is typically between esthetics and retrievability. Eliminating a screw access opening can improve appearance and avoid a hole in a high-wear area, which matters for front teeth and patients with strong bite forces. On the other hand, a crown that is cemented in place can be harder to remove without damage if a repair is needed. For long-term planning, it helps to ask how the restoration would be removed if the crown chips, the abutment loosens, or the implant needs evaluation.
Cement Retained Implants: benefits and real risks to weigh
Cement Retained Implants are a common “screwless” pathway: the implant supports an abutment, and the crown is cemented onto that abutment much like a traditional crown on a natural tooth. This approach can be helpful when implant angulation would place a screw access hole in an undesirable location (such as the front surface of a front tooth). Cement retention may also allow the laboratory to create a crown contour that looks and feels more like a conventional crown.
A widely discussed concern with cemented implant crowns is residual cement left under the gumline. Unlike natural teeth, implants do not have the same connective tissue attachment, and the surrounding tissues can be sensitive to plaque and irritants. If cement is not fully removed, inflammation around the implant can occur and may contribute to peri-implant disease. This does not mean cement retention is “bad,” but it does mean technique matters: margin placement, cement choice, isolation, and cleanup protocols can meaningfully affect risk.
Maintenance is another practical consideration. With a cemented crown, routine checks may focus on tissue health, probing depths as appropriate, radiographs when indicated, and verifying that the bite remains stable. If the crown ever needs to come off, the dentist may need to cut it off, which can add time and cost and may require a new crown. For some patients, that future scenario is acceptable; for others—especially those who value easy repair—retrievability can be a deciding factor.
Restorative Dentistry Implants: planning details people overlook
Restorative Dentistry Implants are not just about placing an implant in bone; the “restorative” side is the entire plan for what the final tooth will look like, how it will be cleaned, and how it will be serviced over time. In a screwless or cement-retained design, small choices early in treatment can have outsized consequences later.
One often-overlooked point is emergence profile—the way the crown comes out of the gum. A bulky contour can trap plaque and make hygiene harder, particularly for back teeth where access is limited. Your dentist may talk about shaping soft tissue, selecting abutment height, and designing the crown’s contour so you can pass floss or interdental brushes without tearing tissue. For U.S. patients with busy schedules, a design that is easier to clean at home can be just as important as how it looks.
Bite forces and material selection also matter. Posterior crowns commonly use zirconia or layered ceramics depending on esthetic needs and opposing teeth. The restoration must withstand chewing forces without creating stress concentrations at the implant connection. In screwless designs, the absence of a screw channel can strengthen some ceramic designs, but retrievability becomes the counterbalance. If you grind your teeth, your dentist may recommend a night guard regardless of retention type to reduce chipping and overload.
Finally, consider how complications are handled. Implants can face issues such as crown fracture, loosening at the abutment screw (even if the crown itself is cemented), food trapping due to contact changes, or tissue inflammation. A clear plan—how the dentist would diagnose the problem and how the restoration would be repaired—should be part of the conversation. Asking “What is the most likely maintenance or repair in five years, and how would you address it?” can surface whether a cemented approach fits your priorities.
In everyday terms, “screwless” can be an esthetic and functional solution, especially when implant angulation makes screw access difficult. The main points to keep in view are tissue health (particularly cement cleanup and margin placement), hygiene access, and the practical realities of repair. When the restorative design matches your bite, cleaning ability, and long-term maintenance expectations, either retention method can be a reasonable choice.




