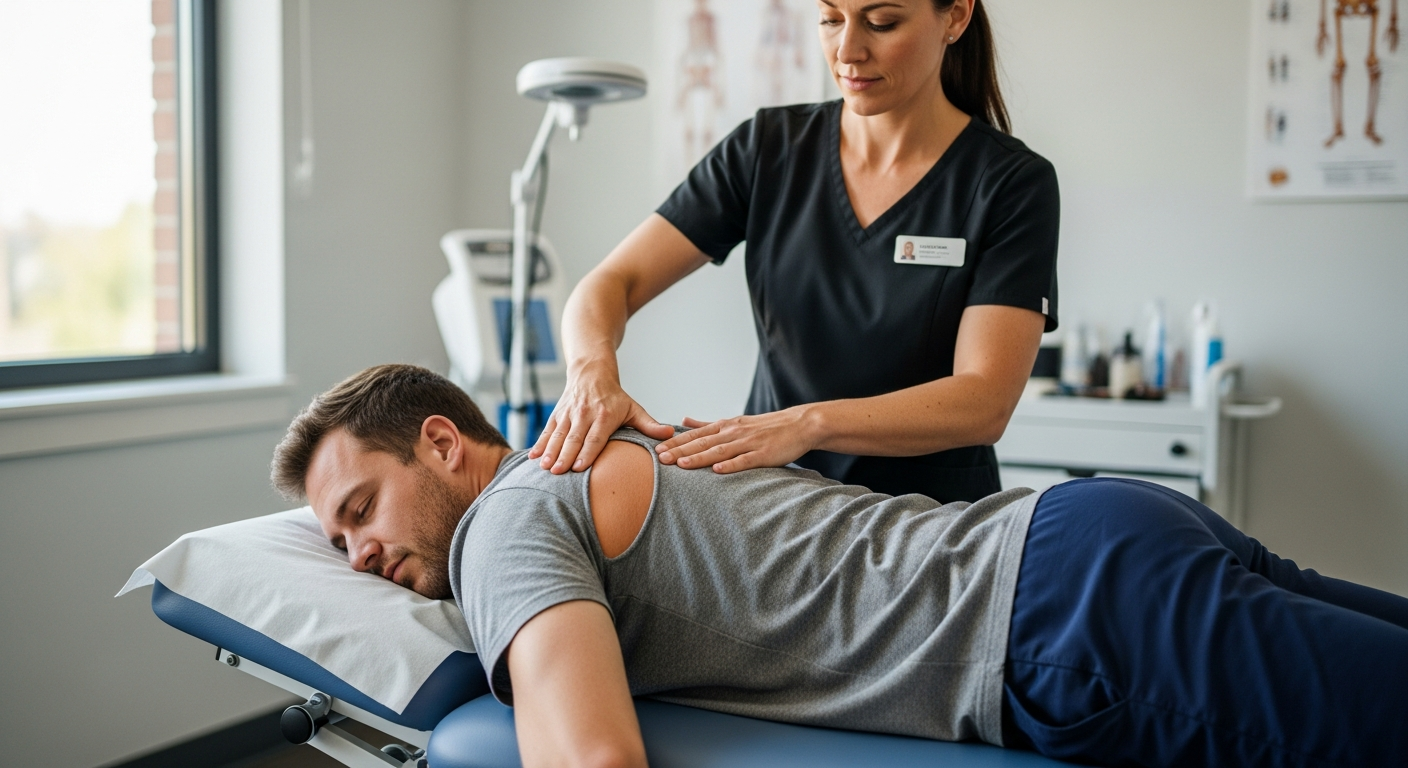
Insights on Managing A1c Levels Effectively
Maintaining healthy A1c levels is a cornerstone of diabetes management and overall metabolic health. This hemoglobin marker provides valuable insight into average blood sugar control over several months, making it an essential tool for both patients and healthcare providers. Understanding what A1c levels mean, how they are measured, and what strategies can help manage them is critical for anyone navigating diabetes or prediabetes. With the right knowledge and resources, individuals can take proactive steps toward better health outcomes and reduce the risk of complications associated with elevated blood sugar.
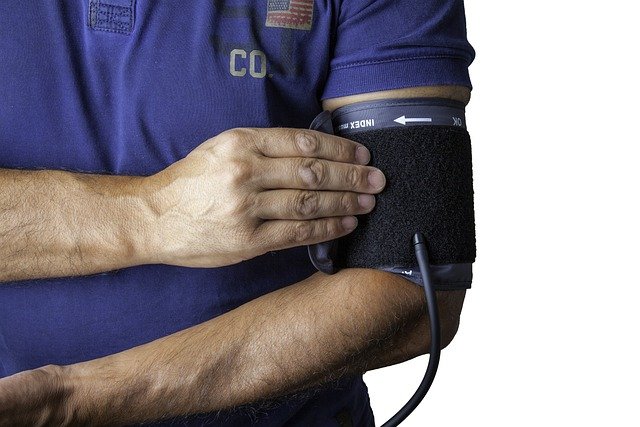
A1c testing has become a standard part of diabetes care, offering a comprehensive view of blood glucose management over time. Unlike daily blood sugar checks that capture single moments, the A1c test reflects average glucose levels over approximately two to three months. This broader perspective helps healthcare providers assess how well treatment plans are working and guides adjustments to medication, diet, and lifestyle interventions.
Understanding A1c Levels
The A1c test measures the percentage of hemoglobin proteins in red blood cells that have glucose attached to them. When blood sugar levels are consistently high, more glucose binds to hemoglobin, resulting in a higher A1c percentage. For individuals without diabetes, a normal A1c level typically falls below 5.7 percent. Prediabetes is generally diagnosed when A1c levels range from 5.7 to 6.4 percent, while diabetes is indicated by an A1c of 6.5 percent or higher. Healthcare providers often set individualized target ranges based on factors such as age, overall health, and the presence of other medical conditions. Regular monitoring allows for timely interventions and helps prevent long-term complications like cardiovascular disease, kidney damage, and nerve problems.
Diabetes Management Resources
Effective diabetes management requires access to reliable resources and support systems. Numerous organizations and healthcare networks provide educational materials, support groups, and tools to help individuals understand their condition and make informed decisions. The American Diabetes Association offers comprehensive guides on nutrition, exercise, medication management, and mental health support. Many hospitals and clinics also run diabetes education programs led by certified diabetes educators who provide personalized guidance. Online platforms and mobile applications have made it easier to track blood sugar levels, log meals, monitor physical activity, and receive reminders for medication or testing. These digital tools often integrate with glucose meters and continuous glucose monitors, providing real-time data that can be shared with healthcare teams. Community support groups, both in-person and virtual, offer emotional support and practical advice from others managing similar challenges.
Find Diabetes Care Options
Accessing quality diabetes care involves finding healthcare providers and facilities equipped to offer comprehensive services. Primary care physicians often serve as the first point of contact, but endocrinologists specialize in hormone-related conditions including diabetes and can provide advanced treatment strategies. Many healthcare systems now offer multidisciplinary diabetes clinics where patients can see physicians, dietitians, pharmacists, and mental health professionals in coordinated visits. Federally Qualified Health Centers and community health clinics provide affordable care options for individuals without insurance or with limited financial resources. Telemedicine has expanded access to diabetes care, allowing patients in rural or underserved areas to consult with specialists remotely. When selecting a provider, consider factors such as experience with diabetes management, availability of diabetes educators, access to advanced monitoring technologies, and the ability to coordinate care with other specialists if needed.
Lifestyle Strategies for A1c Management
Lifestyle modifications play a crucial role in managing A1c levels and improving overall health. Dietary changes often yield significant results, with emphasis on balanced meals that include fiber-rich vegetables, whole grains, lean proteins, and healthy fats while limiting refined carbohydrates and added sugars. Portion control and consistent meal timing help stabilize blood sugar throughout the day. Regular physical activity improves insulin sensitivity and helps cells use glucose more effectively. The American Diabetes Association recommends at least 150 minutes of moderate-intensity aerobic exercise per week, combined with resistance training on two or more days. Weight management is another important factor, as even modest weight loss can lead to meaningful improvements in A1c levels for those who are overweight. Stress management techniques such as meditation, yoga, and adequate sleep also contribute to better blood sugar control by reducing cortisol and other stress hormones that can elevate glucose levels.
Medication and Treatment Approaches
When lifestyle modifications alone do not achieve target A1c levels, medication becomes an important component of diabetes management. Metformin is often the first-line medication for type 2 diabetes, working to reduce glucose production in the liver and improve insulin sensitivity. Other oral medications include sulfonylureas, DPP-4 inhibitors, SGLT2 inhibitors, and GLP-1 receptor agonists, each working through different mechanisms to lower blood sugar. Injectable medications such as insulin may be necessary for type 1 diabetes or advanced type 2 diabetes. The choice of medication depends on individual factors including A1c levels, kidney function, cardiovascular health, and personal preferences. Healthcare providers regularly review medication effectiveness through A1c testing, typically every three to six months, and adjust treatment plans accordingly. Continuous glucose monitors and insulin pumps have revolutionized diabetes management for many patients, providing more precise control and reducing the burden of frequent finger-stick testing.
Monitoring Progress and Preventing Complications
Regular A1c testing is essential for tracking progress and making informed decisions about diabetes management. Most healthcare providers recommend testing every three months for individuals whose treatment has changed or who are not meeting their targets, and every six months for those with stable, well-controlled diabetes. Beyond A1c monitoring, comprehensive diabetes care includes regular screening for complications. Annual eye exams detect diabetic retinopathy before vision loss occurs. Kidney function tests identify early signs of diabetic nephropathy. Foot examinations help prevent ulcers and infections that can lead to serious complications. Blood pressure and cholesterol monitoring address cardiovascular risk factors that are elevated in people with diabetes. Maintaining A1c levels within target ranges significantly reduces the risk of these complications and improves quality of life.
Managing A1c levels effectively requires a comprehensive approach that combines regular monitoring, lifestyle modifications, appropriate medical treatment, and ongoing education. By understanding what A1c levels represent and utilizing available resources, individuals with diabetes can take control of their health and work toward better outcomes. Consistent communication with healthcare providers and commitment to evidence-based strategies form the foundation of successful diabetes management.
This article is for informational purposes only and should not be considered medical advice. Please consult a qualified healthcare professional for personalized guidance and treatment.