Exploring Treatment Choices for Knee Osteoarthritis
Knee osteoarthritis can affect walking, sleep, exercise habits, and confidence in everyday movement. Because symptoms and joint changes vary widely, treatment is usually not one single fix but a combination of steps that reduce pain, protect function, and support long-term joint health.
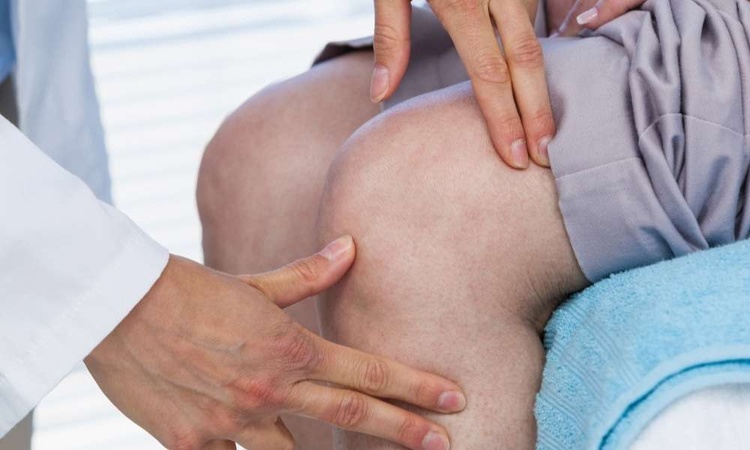
Stiffness, aching, and reduced confidence on stairs are common signs that knee osteoarthritis is affecting daily life. The condition is typically managed with a layered plan: reducing pain and inflammation, improving strength and mobility, and choosing procedures only when simpler measures are no longer enough. The right mix depends on your symptoms, overall health, and goals.
This article is for informational purposes only and should not be considered medical advice. Please consult a qualified healthcare professional for personalized guidance and treatment.
How can you explore treatment choices for knee osteoarthritis?
A practical way to explore treatment choices for knee osteoarthritis is to think in tiers, starting with the least invasive options that still meaningfully improve function. Core building blocks often include activity modification (for example, reducing high-impact moves while keeping regular walking or cycling), targeted exercise to strengthen the quadriceps and hip muscles, and physical therapy focused on gait, range of motion, and balance. Weight management can also reduce knee load; even small changes may affect pain during weight-bearing tasks.
Supportive tools can help you stay active with fewer flare-ups. Depending on alignment and symptoms, a clinician may suggest a knee brace (including unloader braces for certain patterns of wear), a cane used on the opposite side, or shoe inserts. Heat can ease morning stiffness, while ice may help after activity. These options are often combined with medicines or injections when pain limits participation in exercise, which is one of the most important long-term strategies.
Which new medications for osteoarthritis are used today?
When people say they want to discover new medications for osteoarthritis, it helps to clarify what is currently realistic: there is no widely accepted medication proven to reverse knee osteoarthritis or reliably rebuild cartilage once it has worn down. Most drug therapies are aimed at symptom control so you can keep moving, maintain muscle strength, and protect overall function.
Common first-line choices include topical nonsteroidal anti-inflammatory drugs (NSAIDs) applied to the knee, which can reduce pain with less whole-body exposure than pills for some patients. Oral NSAIDs may be appropriate for short periods when risks are acceptable, but they can affect the stomach, kidneys, blood pressure, and cardiovascular risk, so clinicians weigh your history and other medications. Acetaminophen is sometimes used, though its effect is often modest and dosing limits matter for liver safety.
For persistent pain that has a strong nerve or central pain-processing component, duloxetine (a prescription medication also used for certain mood and pain conditions) may be considered by a clinician. Some people are offered short courses of other prescription pain relievers, but opioids are generally approached cautiously because of side effects, dependency risk, and limited long-term benefit for chronic osteoarthritis pain.
Intra-articular injections can also be part of symptom management. Corticosteroid injections may provide short-term relief for inflammation-driven flares, though repeated use needs careful discussion with a clinician. Hyaluronic acid injections are used in some practices, with mixed evidence and variable response from person to person. Platelet-rich plasma (PRP) is offered in some clinics; research is evolving, and protocols differ, so it is important to discuss expected benefit, uncertainty, and safety considerations.
What are effective ways to manage osteoarthritis long term?
To learn about effective ways to manage osteoarthritis over time, focus on habits that keep the knee strong and adaptable. A consistent strengthening plan is often more helpful than occasional intense workouts. Many people benefit from a mix of strengthening (especially quadriceps, hamstrings, glutes), low-impact aerobic activity (cycling, swimming, brisk walking as tolerated), and flexibility work to maintain knee extension and hip mobility. Progression matters: gradual increases reduce flare-ups and improve adherence.
Pain patterns can guide pacing. Using a simple symptom diary (what you did, pain level the next day, swelling) can help you identify triggers and set safe activity thresholds. Flare planning is also useful: short-term rest from aggravating activities, ice, and a return to movement as soon as tolerable usually works better than prolonged inactivity. Sleep, stress, and mood can influence pain sensitivity, so addressing them is part of a complete plan.
When symptoms persist despite conservative care, it may be time to reassess the diagnosis and the joint. Clinicians may check for meniscal tears, inflammatory arthritis, referred pain from the hip or back, or mechanical issues such as significant malalignment. Imaging is not always required early, but it can be helpful when symptoms change, function declines, or a procedure is being considered.
Surgical options are typically discussed only after non-surgical measures have been tried adequately. Arthroscopic “clean-out” surgery is not routinely helpful for typical osteoarthritis, but there are exceptions based on specific mechanical problems. For advanced disease with significant pain and disability, partial or total knee replacement can improve function for many people, though it carries recovery time and risks that should be weighed against expected benefits.
A clear, personalized plan usually includes measurable goals (for example, walking tolerance, stair comfort, return to a hobby), a short list of exercises you will actually do, and a medication or injection strategy tied to function rather than pain alone. Coordinating care among primary care, physical therapy, and orthopedics or rheumatology can help ensure treatments are consistent and adjusted as your needs change.
Long-term knee osteoarthritis management is rarely about finding one perfect treatment. It is more often about combining symptom relief with strength, movement confidence, and periodic reassessment so that the plan matches your life and your knee’s current stage.




