Exploring A1c Levels: What You Need to Know in 2024
A1c testing has become a cornerstone of diabetes management and blood sugar monitoring. This simple blood test provides valuable insight into your average glucose levels over the past two to three months, offering a clearer picture than daily finger-prick tests alone. Whether you're managing diabetes or working to prevent it, understanding what your A1c numbers mean can empower you to make informed health decisions and work more effectively with your healthcare team.
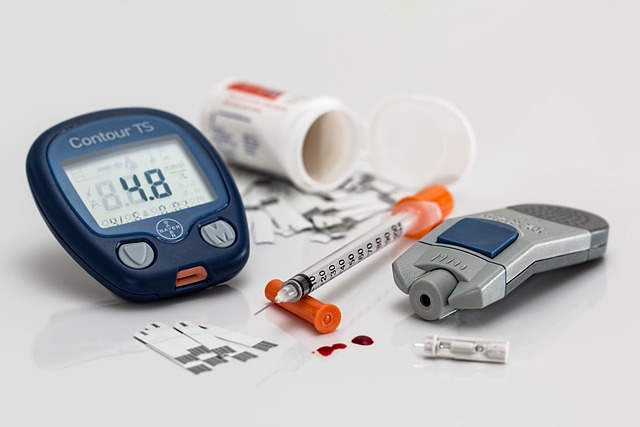
The hemoglobin A1c test measures the percentage of your red blood cells that have glucose attached to them. Since red blood cells live for about three months, this test reflects your average blood sugar levels during that period. For most adults without diabetes, a normal A1c level falls below 5.7 percent. Levels between 5.7 and 6.4 percent indicate prediabetes, while an A1c of 6.5 percent or higher on two separate tests typically confirms a diabetes diagnosis.
Understanding A1c Levels
Your A1c result translates directly to an estimated average glucose level. An A1c of 6 percent corresponds to an average blood sugar of approximately 126 mg/dL, while an A1c of 7 percent indicates an average of about 154 mg/dL. Each percentage point increase in A1c represents roughly a 28-30 mg/dL increase in average blood glucose. Healthcare providers use these numbers to assess how well your current treatment plan is working and whether adjustments are needed. The test requires no fasting and can be performed at any time of day, making it more convenient than traditional glucose tolerance tests. Results are typically available within a few days, though some clinics offer point-of-care testing with results in minutes.
Managing Blood Sugar Levels
Achieving and maintaining target A1c levels requires a comprehensive approach to blood sugar management. For many people with diabetes, the goal is an A1c below 7 percent, though individual targets may vary based on age, overall health, and risk of hypoglycemia. Lifestyle modifications form the foundation of blood sugar control. Regular physical activity helps your body use insulin more efficiently, with both aerobic exercise and strength training showing benefits. Dietary choices significantly impact A1c levels, with emphasis on whole grains, lean proteins, healthy fats, and plenty of vegetables. Portion control and carbohydrate counting help prevent blood sugar spikes after meals. Consistent meal timing and adequate sleep also contribute to more stable glucose levels throughout the day.
Diabetes Monitoring Techniques
While A1c testing provides the big picture, daily monitoring gives you real-time feedback on how food, activity, stress, and medication affect your blood sugar. Traditional fingerstick glucose meters remain widely used, requiring a small blood sample several times daily. Continuous glucose monitors have revolutionized diabetes management by tracking glucose levels throughout the day and night using a small sensor placed under the skin. These devices display current readings, trends, and alerts for high or low blood sugar, allowing for more proactive management. Some systems integrate with insulin pumps to automatically adjust insulin delivery. Keeping detailed records of your readings, meals, physical activity, and medications helps identify patterns and guides treatment adjustments during medical appointments.
How Often Should You Test A1c
Testing frequency depends on your diabetes management status and treatment plan. People with well-controlled diabetes typically test their A1c every six months. If you’ve recently changed medications, aren’t meeting glucose targets, or have type 2 diabetes that isn’t well controlled, your healthcare provider may recommend testing every three months. Those with prediabetes might test annually to monitor progression. Between A1c tests, regular self-monitoring of blood glucose provides ongoing feedback. The frequency of daily testing varies widely based on your treatment regimen. People using insulin may test four or more times daily, while those managing diabetes through diet and oral medications might test less frequently. Your healthcare team will recommend a testing schedule tailored to your specific situation.
Factors That Affect A1c Accuracy
Certain medical conditions can influence A1c results, potentially making them higher or lower than your actual average blood sugar. Anemia, recent blood loss, or blood transfusions can affect red blood cell turnover and skew results. Kidney disease, liver disease, and certain hemoglobin variants may also impact accuracy. Some medications, including high-dose aspirin and certain HIV treatments, can interfere with test results. Pregnancy causes changes in red blood cell production that may affect A1c readings. If you have any of these conditions, your healthcare provider might use alternative tests like fructosamine or glycated albumin, which measure blood sugar control over shorter periods. Always inform your doctor about all medical conditions and medications before interpreting A1c results.
Long-Term Health Implications
Maintaining A1c levels within target range significantly reduces the risk of diabetes-related complications. Studies show that each percentage point reduction in A1c decreases the risk of microvascular complications by approximately 40 percent. Consistently high blood sugar damages blood vessels throughout the body, affecting the eyes, kidneys, nerves, and cardiovascular system. Diabetic retinopathy can lead to vision loss, while kidney damage may progress to kidney failure requiring dialysis. Nerve damage causes pain, numbness, and digestive issues. People with poorly controlled diabetes face increased risk of heart disease, stroke, and peripheral artery disease. Conversely, maintaining good blood sugar control protects these vital organs and systems, supporting better quality of life and longevity. Regular A1c monitoring, combined with comprehensive diabetes care, enables early intervention when levels begin rising.
Understanding your A1c levels empowers you to take an active role in managing your health. Regular testing, combined with daily blood sugar monitoring and healthy lifestyle choices, provides the information needed to prevent or delay diabetes complications. Work closely with your healthcare team to establish personalized A1c targets and develop strategies to achieve them. Remember that A1c is just one tool in diabetes management—it works best when combined with regular medical care, self-monitoring, and attention to overall wellness.




