A1c Levels: Key Insights for Better Health
Understanding A1c levels is crucial for managing diabetes and maintaining optimal health. This important blood test measures your average blood sugar over the past two to three months, providing valuable insights into how well your diabetes management plan is working. Whether you're newly diagnosed or have been managing diabetes for years, knowing what your A1c numbers mean can help you make informed decisions about your health and work more effectively with your healthcare team.
A1c levels serve as a cornerstone measurement in diabetes care, offering a comprehensive view of blood sugar control over an extended period. Unlike daily glucose readings that capture single moments in time, the A1c test provides healthcare providers and patients with a broader perspective on diabetes management effectiveness.
A1c Levels Explained
The hemoglobin A1c test, commonly referred to as A1c or HbA1c, measures the percentage of hemoglobin proteins in red blood cells that have glucose attached to them. Since red blood cells live approximately 120 days, this test reflects average blood sugar levels over the past two to three months. Normal A1c levels for adults without diabetes typically fall below 5.7 percent. Prediabetes is indicated by levels between 5.7 and 6.4 percent, while diabetes is diagnosed when A1c levels reach 6.5 percent or higher.
For most adults with diabetes, the American Diabetes Association recommends maintaining A1c levels below 7 percent. However, individual targets may vary based on factors such as age, overall health, risk of hypoglycemia, and life expectancy. Some people may benefit from more stringent goals below 6.5 percent, while others might have targets of 8 percent or slightly higher.
Tips for Blood Sugar Management
Effective blood sugar management involves multiple strategies that work together to maintain stable glucose levels throughout the day. Dietary choices play a fundamental role, with emphasis on consuming consistent amounts of carbohydrates at regular intervals. Focus on whole grains, lean proteins, healthy fats, and plenty of vegetables while limiting processed foods and sugary beverages.
Regular physical activity significantly impacts blood sugar control by helping muscles use glucose more effectively. Both aerobic exercise and resistance training contribute to improved insulin sensitivity. Even moderate activities like brisk walking for 30 minutes most days of the week can make a meaningful difference in A1c levels.
Medication adherence is equally important for those prescribed diabetes medications. Taking medications as directed, monitoring for side effects, and communicating regularly with healthcare providers ensures optimal therapeutic outcomes. Stress management through techniques like meditation, yoga, or counseling can also positively influence blood sugar control.
Techniques for Monitoring Diabetes
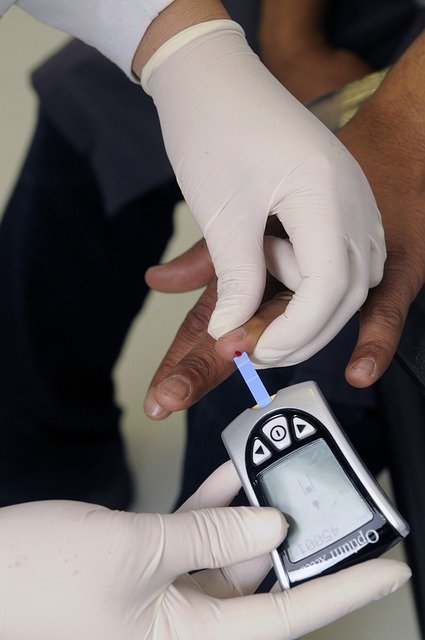
Modern diabetes monitoring encompasses various tools and techniques that provide comprehensive insights into blood sugar patterns. Traditional fingerstick glucose meters remain valuable for spot-checking blood sugar levels, particularly before meals and at bedtime. These devices require small blood samples and provide immediate results.
Continuous glucose monitors represent a significant advancement in diabetes management technology. These devices use small sensors inserted under the skin to measure glucose levels in tissue fluid every few minutes. They provide real-time data, trend arrows showing whether glucose is rising or falling, and alerts for high or low levels.
Keeping detailed logs of food intake, physical activity, medication timing, and glucose readings helps identify patterns and triggers that affect blood sugar control. Many smartphone apps can simplify this process by allowing users to photograph meals, track activities, and sync data from glucose meters or continuous monitors.
| Monitoring Method | Provider/Brand | Key Features | Cost Estimation |
|---|---|---|---|
| Traditional Glucose Meter | OneTouch Ultra 2 | Basic testing, affordable strips | $15-30 for meter, $0.50-1.00 per strip |
| Advanced Glucose Meter | Accu-Chek Guide | Bluetooth connectivity, smartphone app | $20-40 for meter, $0.60-1.20 per strip |
| Continuous Glucose Monitor | Dexcom G7 | Real-time readings, smartphone alerts | $60-70 per month with insurance |
| Flash Glucose Monitor | FreeStyle Libre | 14-day sensors, no finger pricks needed | $35-75 per sensor |
Prices, rates, or cost estimates mentioned in this article are based on the latest available information but may change over time. Independent research is advised before making financial decisions.
Regular A1c testing, typically every three to six months for people with diabetes, provides ongoing feedback about the effectiveness of management strategies. Healthcare providers use these results along with daily glucose monitoring data to adjust treatment plans, modify medication dosages, or recommend lifestyle changes.
Working closely with a diabetes care team that may include endocrinologists, certified diabetes educators, nutritionists, and pharmacists ensures comprehensive support for achieving and maintaining target A1c levels. These professionals can provide personalized guidance, troubleshoot challenges, and help navigate the complexities of diabetes management.
Successful A1c management requires patience, consistency, and ongoing commitment to healthy habits. Small, sustainable changes often produce better long-term results than dramatic short-term modifications. Regular monitoring, professional guidance, and a thorough understanding of how various factors affect blood sugar levels form the foundation for effective diabetes management and improved overall health outcomes.
This article is for informational purposes only and should not be considered medical advice. Please consult a qualified healthcare professional for personalized guidance and treatment.




